What We Do
Minimizing impact, maximizing care with advanced radiation therapy
Dealing with an unexpected medical diagnosis requires taking important initial steps to confidently navigate the situation. At Columbus CyberKnife, we’re here to assist you in understanding your options and finding the best fit for your personal needs.
Whether you’re seeking an alternative to surgery, concerned about the effects of radiation on healthy tissue, or curious about how CyberKnife® can minimize disruptions to your daily life, our goal is to help you discover a treatment plan that suits you.
Our dedicated professionals are experienced in advanced radiation therapy and have access to state-of-the-art technology. We prioritize compassionate and quality care to ensure a comfortable experience. Don’t hesitate to get in touch with the Columbus CyberKnife team to discuss your situation and explore potential solutions.
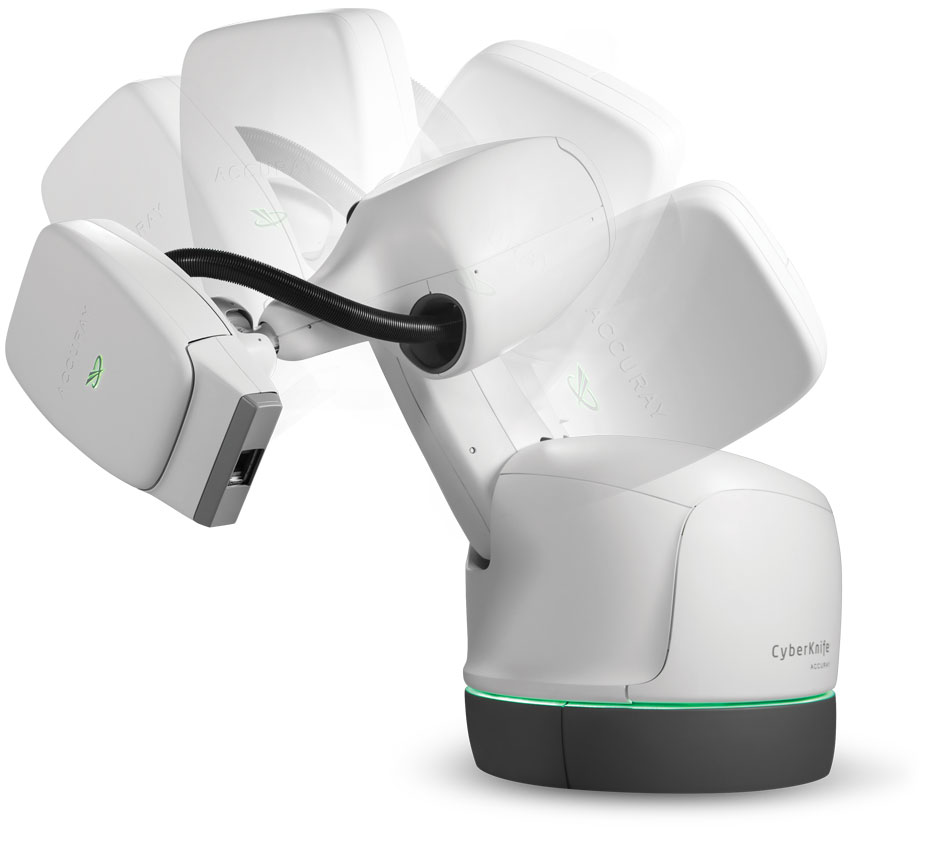
Our Technology
CyberKnife precision delivers a number of unique benefits to patients
Proven Therapy
FDA-approved to treat any part of the body
Safer Treatment
No incisions, anesthesia or hospitalization
Shorter program
1 to 5 visits lasting less than one hour each
Precision Targeted
Surrounding healthy tissues exposed to less radiation


 Douglas W. Widman, MD
Douglas W. Widman, MD Abhay Gokhale, MD
Abhay Gokhale, MD Malolan S. Rajagopalan, MD
Malolan S. Rajagopalan, MD Alexander Masino, MD, PhD
Alexander Masino, MD, PhD Jason Edwin Seavolt, MD
Jason Edwin Seavolt, MD Simeon P. Hodges, III Hodges, III
Simeon P. Hodges, III Hodges, III Erika Stewart, M.S., D.A.B.R.
Erika Stewart, M.S., D.A.B.R. Jenny Porosky, CMD
Jenny Porosky, CMD Christopher Tobolski
Christopher Tobolski Karmin Williams
Karmin Williams Kelsey Ryan
Kelsey Ryan Brittany Rietschlin
Brittany Rietschlin Katie Buck
Katie Buck Margaret Lenaghan, RN, BSN, MS, CHPN
Margaret Lenaghan, RN, BSN, MS, CHPN Lisa Mathews, RN, OCN
Lisa Mathews, RN, OCN

